Platelet Transfusion as Therapy for Endotheliopathy of Trauma
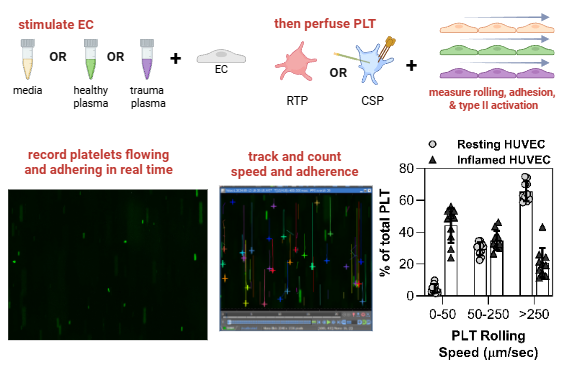
Dysregulation and/or injury of the vasculature, referred to as endotheliopathy, manifests in a disease-specific fashion. The two different platelet transfusion recipient populations outlined above (prophylactic vs. therapeutic) have disparate endotheliopathies which are not well defined. In actively bleeding patients (e.g., hemorrhagic shock), the vasculature is physically damaged, and there is endothelial dysfunction, dysregulated coagulation, and inflammation – collectively referred to as the endotheliopathy of trauma, or EOT. Blood product transfusion is the main source of therapeutic management of hemorrhagic shock, with recent literature suggesting that plasma transfusion is associated with improved endothelial function. Platelets are traditionally transfused to support clot formation in actively bleeding patients, but also possess additional vascular related functions, as described in non-trauma publications: release of soluble mediators to support endothelial function and growth, physical engagement with endothelial cells to restore barrier function, and recruitment and maintenance of endothelial progenitor cells. However, the molecular mechanisms by which platelet transfusions may improve EOT remain poorly understood. We couple microfluidic devices with real time fluorescence microscopy to better understand stored platelet:endothelial interactions under physiologically relevant flow conditions and in the context of the vascular milieu associated with traumatic injury. These studies are focused on identifying key molecular interactions that promote vascular integrity and reduce inflammation, key features of EOT, that may be attributable to or associated with distinct platelet manufacturing and storage conditions.
