Alloimmunization in Response to Transfusion of Novel Platelet Products
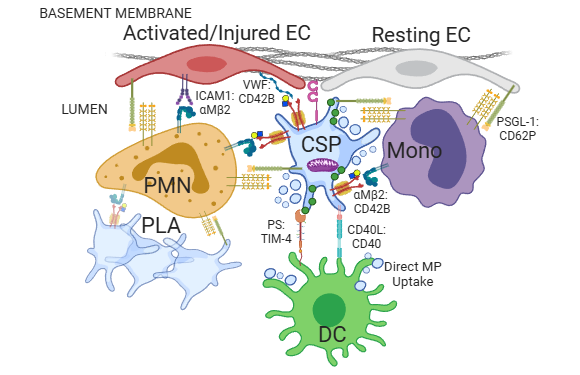
While platelets are most well-known for their hemostatic function (stopping bleeding by forming clots), they also play important roles in pathogen sensing and modulation of innate and adaptive immunity, including antigen presentation. Moreover, platelets are the most allogeneic of all transfused blood products due to the number of polymorphic molecules they express – human platelet antigens (HPA), human leukocyte antigens (HLA), and ABO blood group antigens. This project addresses the urgent need to understand the immune consequences of platelet manufacturing, a significant issue for sensitized patients receiving multiple platelet transfusions. As new platelet products are developed (e.g., pathogen reduced platelets (PR), cold-stored platelets (CSP)), it is necessary to evaluate their safety with respect to alloimmunization. Using these new platelet products and both in vitro and in vivo models, we aim to address how rates of alloimmunization, antigen persistence, and the functional role of platelet:leukocyte aggregates are altered in response to changes in platelet product manufacturing and storage. Long term goals of this project are to determine key molecules involved in maintaining vascular integrity in thrombocytopenic patients versus those key molecules promoting immunogenicity; this will allow for identification of targetable mechanisms to maintain hemostatic function, but limit alloimmune responses after platelet transfusion.
